Medical imaging advances are giving patients more power in their healthcare journeys. This patient-centric approach fosters informed conversations between physicians and patients, increasing adherence to treatment plans.
Modern diagnostic medical imaging modalities offer numerous ways to assess abnormalities both anatomically and functionally, such as Positron Emission Tomography (PET) imaging or ultrasound of cell metabolism.
X-ray
X-rays, an electromagnetic spectrum component, carry enough energy to ionize atoms and break molecular bonds, making X-rays an ionizing radiation that may harm living tissue when exposed over an extended period (for instance during an X-ray exam or certain medical procedures like CT scans or fluoroscopy). However, their benefits often outweigh their minimal risks of exposure.
X-rays differ from other electromagnetic waves in that they can pass unimpeded through bones and dense materials without being absorbed or scattered, which has made X-ray imaging widely utilized in medical diagnostics as well as airport security scanners. Human bodies scanned with X-ray imaging can reveal numerous health problems ranging from broken bones to life-threatening illnesses like cancer.
At an X-ray examination, patients lie on a table while the technologist holds and slides an image receptor or slides the special plate behind an area of interest to take an image. Patients must remain completely still to avoid blurring of the image. Once results have been reviewed by a radiologist, additional images may not be needed and contrast media may be given in drink form to assist the physician in seeing areas within the digestive tract and for other purposes.
All X-ray imaging procedures involve some degree of radiation exposure, though the amount is typically quite minimal. Some procedures, like CT scans and fluoroscopy, may require a higher radiation dose due to multiple images or longer imaging times; the small risk associated with such procedures far outweigh their ability to provide information that could ultimately save lives.
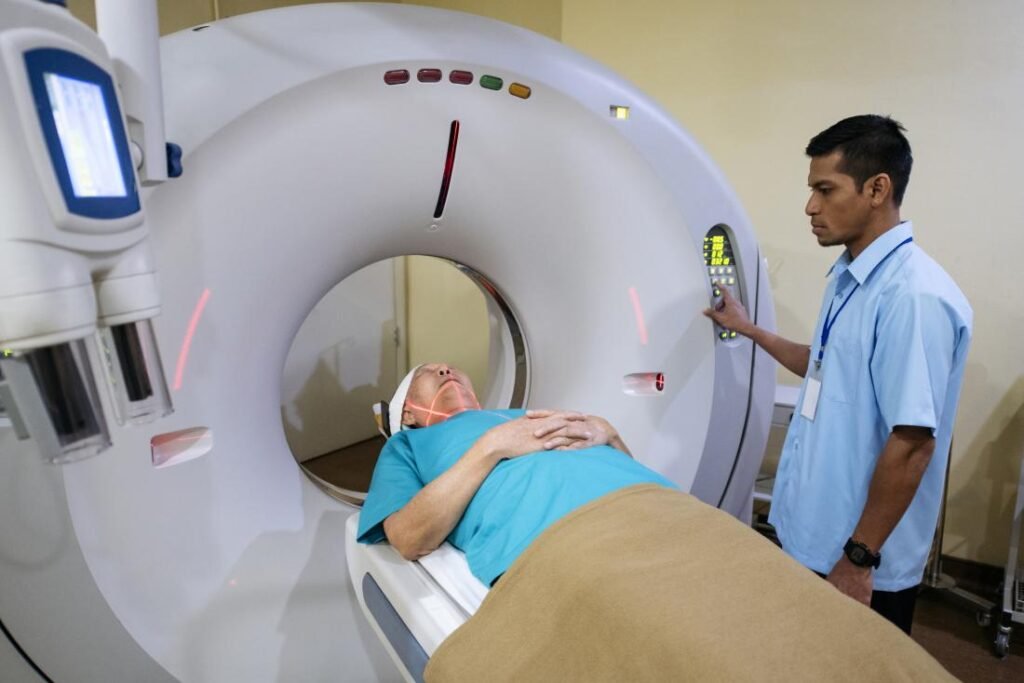
Computed tomography (CT)
Computed tomography (CT scan), or computed tomography, is an imaging technology that uses X-rays and computer technology to produce three dimensional images of internal body structures using X-rays and computer technology. CT scans use these images as diagnostic tools that help physicians detect cancers, infections, injuries and many other medical conditions in a patient’s body; CT scans also allow physicians to see bones, muscles, fat organs and blood vessels within three dimensions and offer valuable insight for surgical planning procedures or surgeries planned.
CT scanners can quickly acquire this information during an emergency situation, often within seconds and fractions of a second. This allows physicians to quickly assess the condition of a patient and focus on any immediate health concerns such as internal bleeding. A CT scan of the chest can identify causes as well as predict whether someone could experience heart attack or stroke symptoms.
CT scans can also be used to image the lungs in order to identify tumors, blood clots and excess fluid accumulation in them. In addition, it’s used to assess vascular aneurysms as well as diagnose lung diseases including emphysema and pneumonia as well as abdominal and pelvic disorders like abscesses or inflammatory bowel disease.
CT scans may also be combined with positron emission tomography (PET) technology, providing both CT’s ability to visualize anatomy and PET’s ability to provide information about cell function and metabolism – helping doctors evaluate certain forms of cancer as well as metabolic disorders like epilepsy. Patients undergoing CT scans should refrain from eating or drinking anything for several hours prior to their exam; additionally they must inform their physician if they have an allergy to any medications, contrast agents, Betadine soap or latex products.
Magnetic resonance imaging (MRI)
Magnetic Resonance Imaging (MRI) employs powerful magnets and radio waves to produce clear and detailed images without using radiation-emitting sources, making it especially well-suited to imaging soft tissue such as nerves, spinal cord, muscles and connective tissue in the body. Furthermore, its exceptional spatial resolution enables it to visualize structures within bone or cartilage structures.
MRI can also be an invaluable asset in diagnosing brain tumours and aneurysms, through techniques like functional Magnetic Resonance Imaging (fMRI). With these specialized MRI techniques, doctors are able to observe brain activity by watching how different parts of the brain react during specific tasks.
An MRI scan produces images of thin slices taken of the body from various directions: top (axial), front (coronal), and sides (sagittal). Your doctor may inject contrast dye into your bloodstream to highlight specific tissues; gadolinium-containing dye has magnetic properties and absorbs into some tissues while being rejected from others; these images can then be used to help diagnose conditions like musculoskeletal issues, brain tumours, infections of joints or inflammation of ligaments and more.
MRI involves the use of high-power magnets which may interfere with certain medical devices such as heart pacemakers or metallic implants such as clips. Therefore, it is crucial that any potential patients with metal implants or heart pacemakers inform their physician prior to having an MRI done; in some cases lead aprons will also be necessary.
Ultrasound
Ultrasound (US) utilizes sound waves to produce images of internal body structures without using radiation, offering significant health advantages over its more irradiant alternative, X-ray. US can assess organ and tissue conditions without touching them directly and without risking harm to patients or medical experts alike. However, ultrasound has some restrictions and should only be utilized when necessary – it cannot view bones and is unsuitable for examining tissues with air content such as lung tissue and the fetus.
To conduct an ultrasound examination, a transducer (probe) must be placed on the skin. Although it’s usually noninvasive, an ultrasound probe can also be placed inside vagina for pelvic exams; or in their rectum for prostate and sexology exams; or even their oesophagus for cardiovascular and urology exams.
Ultrasound imaging provides a real-time view of internal organ structures and their movements, including that of an unborn fetus in pregnancy scans. Ultrasound can also guide invasive procedures like biopsies or biopsy procedures and detect whether a lump is cancerous or simply fluid-filled cyst.
Ultrasound can be performed in hospitals, imaging centers, doctor’s offices and other health care facilities. While typically painless, ultrasound testing can become uncomfortable if being scanned is painful or sensitive. Therefore, it’s essential that you follow all instructions from healthcare providers for prepping for an ultrasound – including refraining from certain foods and medications, changing into a hospital gown and understanding what the results indicate about your health and wellbeing – normal results indicate your organs are functioning normally and provide invaluable information for doctors while abnormal results could indicate something is amiss which requires further investigation from health care facilities or further testing from laboratories.
Artificial intelligence (AI)
AI uses machine learning to analyze medical imaging data and assist healthcare professionals in recognizing abnormalities. AI also aids healthcare providers with interpreting results and improving patient care; providing faster and more accurate diagnoses than traditional methods; it can assist physicians with recognizing cardiovascular conditions, fractures and musculoskeletal injuries and developing targeted treatments; it may even identify causes for chronic diseases and provide targeted solutions.
AI can revolutionize medicine. Its potential benefits include expedited drug discovery, accurate diagnoses and reduced costs; however, for maximum impact it must be tailored specifically to each medical context and tested to ensure its safety and efficacy.
AI excels at repetitive and detail-oriented tasks, freeing physicians to focus on more complex cases. Furthermore, AI can reduce diagnosis time to prevent workplace burnout as well as enhance overall healthcare outcomes by decreasing human mistakes.
One of the greatest difficulties associated with AI medical imaging is processing large volumes of data that it must analyze from various institutions – this may lead to inaccurate prediction results and lead to additional processing time and resources being expended on processing it all.
AI algorithms present the risk of bias and discrimination. Therefore, it is crucial that radiology professionals remain mindful of this potential for discrimination by AI algorithms, and understand its potential effects. Collaboration between clinicians and engineers to ensure safe technology for patients should take place, with stringent evaluation criteria and reporting guidelines for AI applications in medicine being developed – this will prevent unintentionally or intentionally creating biased or discriminatory systems from emerging.

